1494
Views & Citations494
Likes & Shares
Alkaptonuria is a rare autosomal recessive metabolic disease caused by
homogentisic acid oxidase enzyme deficiency. High homogentisic acid levels will
eventually result in black deposits in skin, sclerae, connective tissues
(ochronosis) and urine (alkaptonuria). It can lead to early degeneration of
joints. The diagnosis is often delayed because of its low prevalence and
non-specific early symptoms. We describe a clinical presentation of ochronotic
arthropathy, on a complex patient, who developed a septic arthritis of the
knee. The patient was under immunosuppressive therapy, due to a previous colon
adenocarcinoma and received a knee corticosteroid infiltration, two weeks
before the onset of pain. It was performed joint lavage and arthrolysis by
arthrotomy. During the procedure, we found a dark pigmentation on bone. Urine
tests were positive for alkaptonuria. The patient completed an antibiotic cycle
and rehabilitation, with satisfying improvement in knee’s range of motion. At
four years follow-up the patient can walk without crutches, presents minor knee
pain. High level of suspicion and awareness is needed to diagnose ochronosis.
The joint destruction in a complex patient must be carefully analysed. We have
chosen a non-aggressive therapeutic management, but according to the
literature, other therapeutic strategies could have also been chosen, like
joint arthroplasty. We’ve declined this option because the patient is still
doing antineoplastic treatment.
INTRODUCTION
Alkaptonuria is a rare autosomal recessive
metabolic disease, with an incidence of 1:125,000 to 1:1 million worldwide.
First description of Alkaptonuria was done by Garrod in 1908 that also
recognized it to follow classic Mendelian recessive inheritance. The genetic
defect is mapped to the HGD gene and more than 90 different mutations have been
identified to date. Alkaptonuria is caused by homogentisic acid oxidase enzyme
deficiency that results in high homogentisic acid levels. It will eventually
result in black deposits in skin, sclera, connective tissues and urine.
Ochronosis, dark pigmentation of connective tissues, is the musculoskeletal
manifestation of this disease [1-3]. It can lead to early degeneration of
cartilage, leading to secondary osteoarthritis, by a mechanism that has not
been understood. A worldwide review conducted in 2004 found that approximately
600 cases of ochronotic arthropathy have been reported since 1962. The
diagnosis is often delayed because of its low prevalence and non-specific early
symptoms. The diagnosis occasionally is discovered intraoperatively in patients
undergoing joint replacement surgery through the observation of the
characteristic bluish-black pigmentation of the tissue surrounding the joint.
Ochronotic arthropathy manifests first in the spine. Subsequent degeneration is
on the knee (most commonly affected, in 64% of cases), hip and shoulder [4].
Small joints of the hand and foot usually are not affected. Homogentisic acid
and its oxidation products could accumulate also in the sclera, skin, heart
valves, the cartilage of the nose and ears, tendons, ligaments, renal tubule
epithelial cells, pancreas and arteries [5-7]. In this paper, it is described a
clinical presentation of ochronotic arthropathy with septic arthritis in the
knee, of a complex patient.
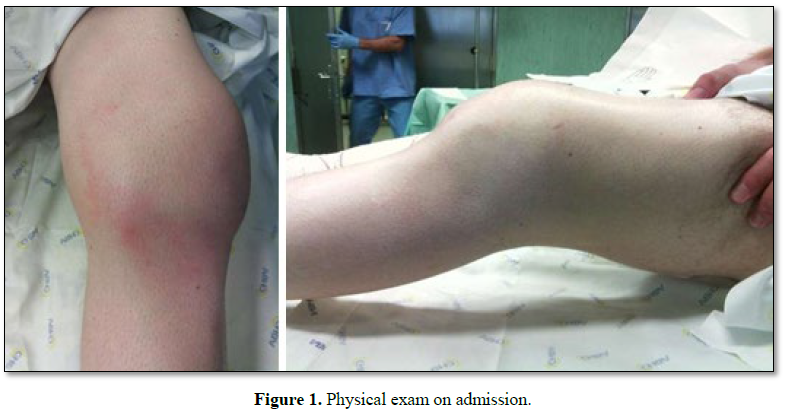
CLINICAL CASE
DISCUSSION
The diagnosis of alkaptonuria may be suspected by an accurate physical
examination. Dark pigmentation on sclera and on ear cartilage is typically
described [6], but not so easy to find in these patients. The classic clinical
triad of alkaptonuria is homogentisic aciduria, ochronosis and ochronotic
arthropathy [7]. Overall, the incidence of ochronotic arthropathy in patients
with alkaptonuria is low [2]. Antimalarial treatment and use of skin-creams
containing hydroquinone are important differential diagnosis with exogenous ochronosis
[8]. Differential diagnosis must be done with ankylosing spondylitis and
degenerative osteoarthosis [7]. However, certain radiologic findings allow its
differentiation, like unusual sites of joint involvement (severe glenohumeral
joint disease in the absence of significant trauma, advanced changes in the
sacroiliac joints and symphyseal joints), and joint-space loss with an unusual
pattern (symmetrical joint-space narrowing in the hips and shoulders, and
isolated lateral femorotibial loss of knee joint space) (Figure 4). Involvement of large peripheral joints usually occurs
about 10 years after spinal changes [7]. Darkening of the urine is a common
diagnostic feature and should be considered in children even producing it
unusually [2]. Diagnosis can be confirmed using gas liquid chromatography,
thin-layer chromatography, or enzymatic spectrophotometry to analyse the amount
of homogentisic acid in the patient’s urine. Arthroscopy has been found to be
an effective diagnostic tool in cases of suspected ochronosis [2].
For septic arthritis, it is strongly recommended immediate antibiotic
therapy and evacuation of purulent material as often as necessary. However, few
published data are available that addresses the most effective methods of
evacuating this purulent material. Gächter et al. [9] defends that the degree
of debridement required according to the intraoperative stage of the joint. Our
open approach was based on bad clinical stage of the high-risk patient and
radiographic osteolysis, classifying in stage IV. In these cases, open
arthrotomy is recommended to effectively eradicate the infection in one-time
surgery, with debridement, removal of loose fragments and curettage the cysts.
When patients’ symptoms lasting four to ten days, Kirchhoff et al. [10] treated
them by open surgery or were converted from arthroscopy to open debridement due
to advanced stages. Arthroscopic treatment is also indicated with septic
arthritis on native knees with low reinfection rate and good functional
outcomes [11]. Although, Aim et al. [12] showed that 25% required more than one
arthroscopic lavage and factors significantly associated with arthroscopic
treatment failure were Gächter stage III or IV and positive drainage-fluid
cultures after 24 h. It’s consensual that all incisions must be closed
completely (no drains) and an aggressive early range of motion postoperatively
must be routinely emphasized. Another controversy theme is the empiric
antibiotic. Current antibiotic choices should be made based on the likely
etiological organisms (geographic variation and resistance patterns) and
subsequently modified in light of culture and sensitivity results. Our choice
is justified by UK guidelines on initial antibiotic choice [13]. Fusidic acid
may also be considered as an adjunct because of apparently good penetration
into bone [13]. Although it should be noted that MRSA is gradually emerging and
has been recently reported a prevalence of up to 17% [10]. With regard to the
choice of antibiotic, a multidisciplinary approach with microbiologists is
essential.
Currently, there is no proven therapy or prophylactic treatment for
alkaptonuric patients [2,4]. Treatment options are administration of
non-steroidal anti-inflammatory drugs, intake of preparations containing
glucosamine and chondroitin sulphate, intra-articular injection of hyaluronic
acid and steroids, arthroscopic debridement of the affected joint and
arthroplasty. Treatment is generally supportive and aimed at preventing or
minimizing the effects of ochronotic arthropathy, like others arthritis. More
specific, the antioxidant properties of vitamin C have been shown to help slow
the conversion of homogentisic acid to its pathologic polymeric intermediate
[2,6]. Dietary restrictions of foods containing phenylalanine and tyrosine have
been shown to be effective in limiting symptoms of ochronotic arthritis because
this reduces the production of homogentisic acid. Vitamin E and N-acetyl
cysteine are potential therapies because of their scavenging of free radicals
and consequent limitation of oxidative damage to joint tissue [2]. The drug
nitisinone is being researched as the first potential treatment for
alkaptonuria; in previous research it was shown to reduce the levels of HGA by
up to 95% [6]. In our patient, we focus the challenge to decide which tissue
were infected or simply with dark pigmentation. Sometimes it was difficult to
know until where we should do the debridement. This is the second case
described in literature with infection and ochronosis, but there not seems to
have any relationship between them [4]. The immunocompromised system and
injection on the knee must have acted as risk factors for septic arthritis in
this case. The joint destruction in these complex patients (with
adenocarcinoma, ochronosis arthropathy and septic arthritis) was analysed
carefully and it was chosen a non-aggressive management. Other therapeutic
strategies could also have been considered according to the literature.
Arthroplasty performed in patients with ochronotic arthropathy suggests that
the procedure is effective in the alleviation of joint pain and the improvement
of mobility [2], even in shoulders [3]. However, it was declined this option
because he is still doing antineoplastic treatments, and there is no benefit in
some surgery or even infiltration. About prognosis, patients with alkaptonuria
can expect a normal life.
Nevertheless, the complications of debilitating arthritis, chronic
kidney disease and ochronotic skin alterations will occur [6].
CONCLUSION
1. Lal
M, Thakur m, Kashyap S (2014) Alkaptonuric ochronosis. Orthopedics 37: e1141-11149.
2. Gil
JÁ Wawrzynski J, Waryasz GR (2016) Orthopedic Manifestations of ochronosis:
Pathophysiology, presentation, diagnosis and management Am J Med 129: 536.e1-e6.
3. Drakoulakis
E, Varvitsiotis D, Psarea G, Feroussis J
(2012) Ochronotic arthropathy: Diagnosis and management: A critical review. Am
J Orthop (Belle Mead NJ) 41: 80-83.
4. Jasper
J, Metsaars W, Jansen J (2016) Ochronosis of the knee with secondary
osteoarthritis requiring total knee replacement in a patient with cryptogenic
organising pneumonia. BMJ Case Rep 2016: bcr2016215412.
5. Karaoglu
S, Karaaslan F, Mermerkaya MU (2016) Long-term result of arthroplasty in the
treatment of a case of ochronotic arthropathy. Acta Orthop Traumatol Turc 50: 584-586.
6. Couto
A, Sá Rodrigues A, Oliveira P, Seara M (2018) Ochronotic arthropathy – A rare
clinical case. Oxford Med Case Rep 2018: 302-305.
7. Ventura-Ríos
L, Hernández-Díaz C, Gutiérrez-Pérez L, Bernal-González A, Pichardo-Bahena R, et
al. (2014) Ochronotic arthropathy as a paradigm of metabolically induced
degenerative joint disease. A case-based review. Clin Rheumatol 35: 1389-1395.
8. Levin
CY, Maibach H (2001) Exogenous ochronosis. An update on clinical features, causative
agents and treatment options. Am J Clin Dermatol 2: 213-217.
9. Stutz
G, Kuster MS, Kleinstück F, Gächter A (2000) Arthroscopic management of septic
arthritis: Stages of infection and results. Knee Surg Sports Traumatol Arthrosc
8: 270-274.
10. Kirchhof
C, Braunstein V, Buhmann S, Oedekoven T, Mutschler W, et al. (2009)
Stage-dependant management of septic arthritis of the shoulder in adults. Int
Orthop 33: 1015-1024.
11. Bohler
C, Dragana M, Puchner S, Windhager R, Holinka J (2016) Treatment of septic
arthritis of the knee: A comparison between arthroscopy and arthrotomy. Knee
Surg Sports Traumatol Arthrosc 24: 3147-3154.
12. Aim F,
Delambre J, Bauer T, Hardy P (2016) Efficacy of arthroscopic treatment for
resolving infection in septic arthritis of native joints. Orthoped Traumatol Surg
Res 101: 61-64.
13. Ateschrang
A, Albrecht D, Schroeter S, Weise K, Dolderer J (2011) Current concepts review:
Septic arthritis of the knee pathophysiology, diagnostics and therapy. Wien
Klin Wochenschr 123: 191-197.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Journal of Cancer Science and Treatment (ISSN:2641-7472)
- Journal of Pathology and Toxicology Research
- Journal of Nursing and Occupational Health (ISSN: 2640-0845)
- Chemotherapy Research Journal (ISSN:2642-0236)
- Journal of Infectious Diseases and Research (ISSN: 2688-6537)
- Journal of Allergy Research (ISSN:2642-326X)
- BioMed Research Journal (ISSN:2578-8892)